The current US Department of Agriculture (USDA) Recommended Daily Allowance (RDA) for iodine is 150 mcg for adolescents and adults. Why do so many in the iodine community, including health professionals, take 12.5 mg or more which is 87 times the USDA Iodine RDA?
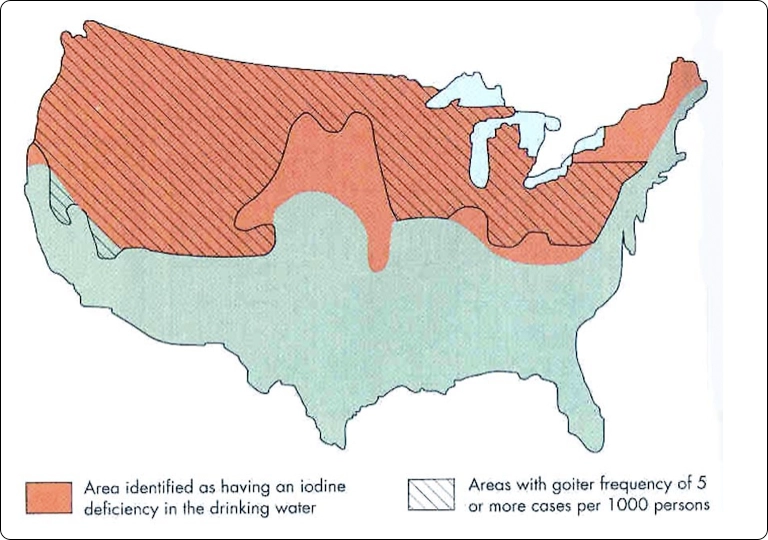
Iodine has always been an important part of our diet. However, in North America we only began to appreciate its importance in the early 1900s.[1] Landlocked areas in the US and southern Canada, from the Rockies to New York, experienced an epidemic of goiter. Goiter is the swelling of the thyroid which allows it to absorb as much iodine from the blood as possible. Areas close to the sea has iodine rich water, air, soil and food. The Goiter Belt, most of which is well inland, has very little iodine in the environment.
The Canadian and US governments started adding iodine to salt and other foods to solve the epidemic. At the time it was believed that 2 mg of iodine was toxic for the human body and the recommendation was set well below that level. In the 1950’s the USDA set the RDA at only 150 mcg which was sufficient to address the goiter problem. At that time iodine could be found in bread, as it was added to the yeast as a preservative.[2, 3] It was also added to salt to ensure the population was getting enough iodine for preventing goiter. Later, iodine in bread was replaced by bromine, a halide which competes with iodine for receptor sites in the body.
Adding iodine to regular foods solved the goiter problem, but it did not solve iodine deficiency. Iodine deficiency had not yet been well measured and understood.
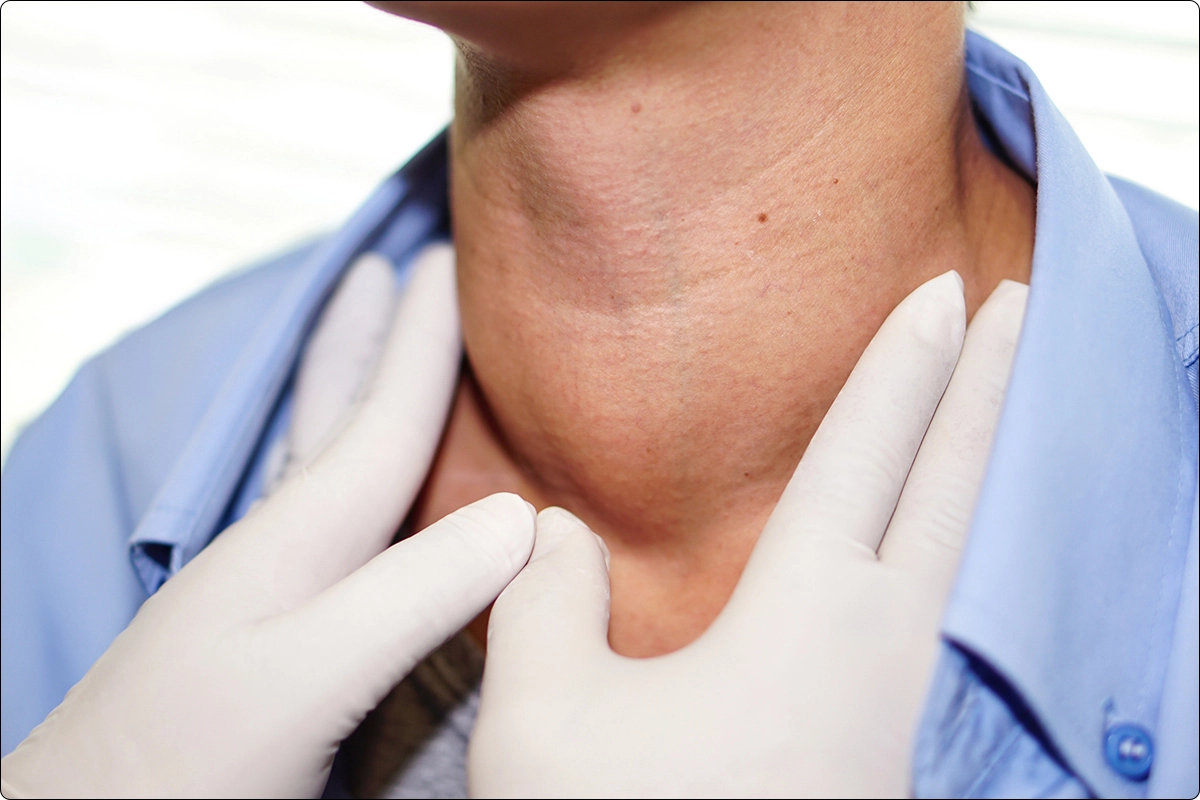
Nowadays doctors and the public are beginning to realize the importance and benefits of taking sufficient iodine for the entire the body. They recognize that the recommended daily amount is not nearly enough to restore optimal health in the body. Most users take 12.5 mg and it is becoming more common for users to take 25 mg, 50 mg, 100 mg and more without experiencing harmful side effects.
Researchers have estimated the body stores about 1500 mg of iodine, of which about 50 mg is stored in the thyroid. Cells that concentrate iodine include the thyroid, muscle tissue, white blood cells[4], salivary glands, eye glands and muscles, kidney cells, the pancreas, lungs[5], liver, nasal passage, cerebral brain fluid, blood vessels in the brain, skin, adrenals, testicles[6, 7], thymus gland[8], ovaries[9], placenta and uterus[10, 11].
Some users take larger doses at the beginning of supplementation to restore the body to optimal function. These larger doses allow the body to better displace toxic halides from iodine receptor sites and restore iodine levels in tissues, including breast tissue. This can reduce the risk of cancer in the breast, prostate and in other parts of the body.
Iodine is an essential component of total body health. The Zen Haus Dual Form Iodine Supplement is labelled ‘High Potency’ because it provides 12.5 mg of elemental iodine per tablet. Much higher than the USDA Iodine RDA. It is what prominent iodine doctors and researchers recommend as a maintenance amount for total body supplementation.
.
.






